Understanding Pyoderma Gangrenosum: Symptoms, Causes, and Treatment
Introduction Pyoderma Gangrenosum

Pyoderma Gangrenosum is a rare and perplexing skin condition that can be debilitating for those affected. In this comprehensive guide, we will explore the essential aspects of Pyoderma Gangrenosum, including its symptoms, potential causes, available treatment options, and the challenges individuals face while living with this condition.
Unraveling Pyoderma Gangrenosum: Pyoderma Gangrenosum, commonly abbreviated as PG, is a perplexing skin disorder characterized by the development of large, painful ulcers on the skin, primarily affecting the legs. While the precise origin of pyoderma gangrenosum remains shrouded in mystery, it is believed to emerge from a malfunction in the body’s immune system. This condition is also recognized for its associations with specific diseases, adding to its enigmatic nature.
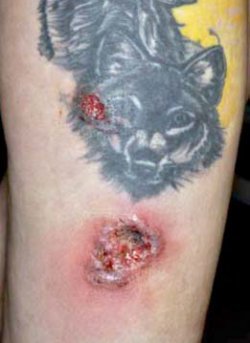
Symptoms of Pyoderma Gangrenosum: The hallmark symptom of Pyoderma Gangrenosum is the emergence of skin ulcers. These ulcers can manifest anywhere on the body, but they predominantly appear on the lower extremities, especially the legs. They exhibit distinctive features such as rapid growth, intense pain, and a unique purple or blue border. In some cases, these ulcers may exude pus or other fluids, further exacerbating the discomfort experienced by individuals grappling with this condition.
Pyoderma gangrenosum, a rare skin condition, leads to the development of large and painful skin ulcers, primarily affecting the legs. While the exact underlying causes of pyoderma gangrenosum remain mysterious, it is thought to be associated with an immune system malfunction. Furthermore, this condition often presents in conjunction with inflammatory bowel disease and is characterized by the presence of painful pustules on the arms and legs. These pustules gradually progress into open sores. Physicians identify pyoderma gangrenosum based on specific diagnostic criteria referred to as the “5 P’s of PG”:
- Painful
- Progressive
- Purple
- Pretibial
- Pathergy
These diagnostic parameters can be observed during the initial evaluation of a patient with pyoderma gangrenosum, obviating the need for histopathology, laboratory findings, or treatment responses as sole criteria for diagnosis
Probing the Causes
The exact etiology of Pyoderma Gangrenosum remains an enigma. It is widely classified as an autoimmune disorder, signifying that the body’s immune system mistakenly launches an assault on healthy skin tissue. Certain triggers, such as physical injury or surgical procedures, may catalyze the development of Pyoderma Gangrenosum in susceptible individuals. Furthermore, there exists compelling evidence of a genetic predisposition to this perplexing condition.
Pathophysiology

Pyoderma gangrenosum presents a formidable diagnostic and treatment challenge due to its multifaceted origin. This rare skin condition is typically identified through clinical assessment, ruling out factors such as infection, neoplasia, thrombophilia, and various inflammatory disorders. There is a scarcity of research on its underlying causes and treatment options. Anomalies in the functionality of inflammatory cytokines, the immune system, and neutrophils, coupled with specific genetic mutations, increase the susceptibility to this intricate ailment. Enhancing the early detection of individuals at risk of pyoderma gangrenosum and refining its timely diagnosis are pivotal for the potential development of targeted and personalized therapeutic approaches. A deeper understanding of pyoderma gangrenosum’s intricate pathogenesis holds the key to its future outlook.
Diagnosing the Enigma: Diagnosing Pyoderma Gangrenosum is no straightforward feat, as its symptoms can closely mimic those of other dermatological conditions or infectious skin ailments. Dermatologists and healthcare providers conduct a meticulous assessment of the skin and frequently resort to supplementary diagnostic measures to eliminate alternative diagnostic possibilities. Biopsies, blood tests, and skin cultures are among the customary tools employed in establishing an accurate diagnosis.
Treatment Options:
While an outright cure for Pyoderma Gangrenosum remains elusive, a spectrum of treatment options exists to mitigate its impact and facilitate the healing process. These therapeutic avenues encompass:
- Medications: Physicians often prescribe immunosuppressive medications, such as corticosteroids and biologics, to curb the immune system’s hyperactive response and quell inflammation.
- Wound Care: Prudent wound management is imperative to avert infection and expedite the healing process. This entails the application of specialized dressings, antibiotics, and diligent wound cleansing.
- Surgical Intervention: In certain instances, surgical intervention may prove necessary to excise damaged tissue or close extensive ulcers.
- Pain Management: Alleviating the distress associated with Pyoderma Gangrenosum is of paramount importance. Medical practitioners may deploy pain-relief medications and employ various techniques to address this facet of the condition.
Resilience and Quality of Life
Living with Pyoderma Gangrenosum is a challenging ordeal that not only exacts a physical toll but also takes an emotional and psychological toll on affected individuals. A robust support network comprising healthcare professionals and emotional support from friends and family is indispensable. Coping strategies and adjustments to one’s lifestyle can significantly enhance the quality of life for those grappling with this condition.
for more article
Summary
Pyoderma Gangrenosum remains a rare and enigmatic skin condition that can profoundly impact the lives of those afflicted by it. While an absolute cure remains beyond reach, timely diagnosis and appropriate management strategies hold the key to controlling symptoms and promoting healing. If you suspect that you may be dealing with Pyoderma Gangrenosum, it is imperative to seek medical attention from a dermatologist or healthcare provider who can provide an accurate diagnosis and devise a tailored treatment plan. Pyoderma Gangrenosum is an enigma that continues to challenge the medical community, but with diligence and unwavering support, individuals can navigate its complexities and embark on a path to healing and improved well-being
- Rare Skin Condition: Pyoderma Gangrenosum is a rare and perplexing skin disorder that leads to the development of painful and rapidly progressing skin ulcers.
- Painful Ulcers: The primary symptom is the formation of skin ulcers, which can appear anywhere on the body but are commonly found on the legs. These ulcers are known for their rapid growth and intense pain.
- Autoimmune Connection: Pyoderma Gangrenosum is believed to be an autoimmune disorder, where the body’s immune system mistakenly attacks healthy skin tissue.
- Triggers and Genetic Predisposition: Certain triggers, such as injury or surgery, may lead to the development of Pyoderma Gangrenosum in susceptible individuals. There is also evidence of a genetic predisposition to the condition.
- Diagnostic Challenges: Diagnosing Pyoderma Gangrenosum can be challenging due to its symptoms resembling those of other skin conditions. Dermatologists often rely on a combination of clinical examination, biopsies, blood tests, and skin cultures for an accurate diagnosis.
- No Definitive Cure: There is no known cure for Pyoderma Gangrenosum, but several treatment options are available to manage the condition and promote healing.
- Treatment Options: Treatment may include medications to suppress the immune response, wound care to prevent infections, and, in some cases, surgical interventions to remove damaged tissue.
- Pain Management: Managing the pain associated with Pyoderma Gangrenosum is crucial, and healthcare providers employ various methods for pain relief.
- Emotional and Social Support: Individuals living with Pyoderma Gangrenosum often require emotional and social support to cope with the physical and psychological challenges posed by the condition.
- Quality of Life: While Pyoderma Gangrenosum can be debilitating, timely diagnosis and appropriate management can help control symptoms and improve the quality of life for those affected.